According to the World Bank (2019), malnutrition leads to more than 10% potential reduction in lifetime earnings for each malnourished individual. If we count the total loss due to malnutrition in a country, the GDP loss would stand at about ≥ 2 to 3%.
The combination of malnutrition and lack of access to primary healthcare, water, sanitation and hygiene is responsible for poor health and various non-communicable diseases. These affect a person’s entire lifecycle from childhood to productive years to advanced age. Together, they result in early mortality, low productivity and increased health cost, trapping extremely poor households into lifelong financial hardships.
PKSF’s Pathways to Prosperity for Extremely Poor People (PPEPP) project seeks to tackle this particular development challenge in a lifecycle approach. In line with the National Nutrition Policy (NNP-2015) and National Plan of Action for Nutrition (NPAN-2), the FCDO and EU-funded project is working in three broad areas:
a) Delivery of a package of essential services either by supporting better delivery of the National Nutrition Services (NNS) or through direct delivery where there are significant gaps in NNS capacity;
b) Community-level work to address some of the social practices that prevent good nutrition outcomes; and
c) Promoting nutrition-sensitive income-generating activities (IGAs) that support nutrition outcomes.

Prosperity’s primary health, nutrition and WASH services cover more than 200,000 extremely poor households, with special focus on infants, under-5 children, expecting and lactating mothers, adolescent girls, women of childbearing age, the elderly and persons with disability. The project takes its nutrition-specific, nutrition-sensitive, referral and linkage-building services to the doorsteps of participant households and the larger community.
Our grassroots primary health and nutrition campaigns build awareness on nutrition, health and WASH both at service seeker level and the service provider level. Our 257 trained health workers provide technical support for establishment of nutrition-sensitive IGAs in the community to ensure better nutrition intake for healthier life. This is directly linked to higher productivity, consumption gains and improved living conditions of the target households.
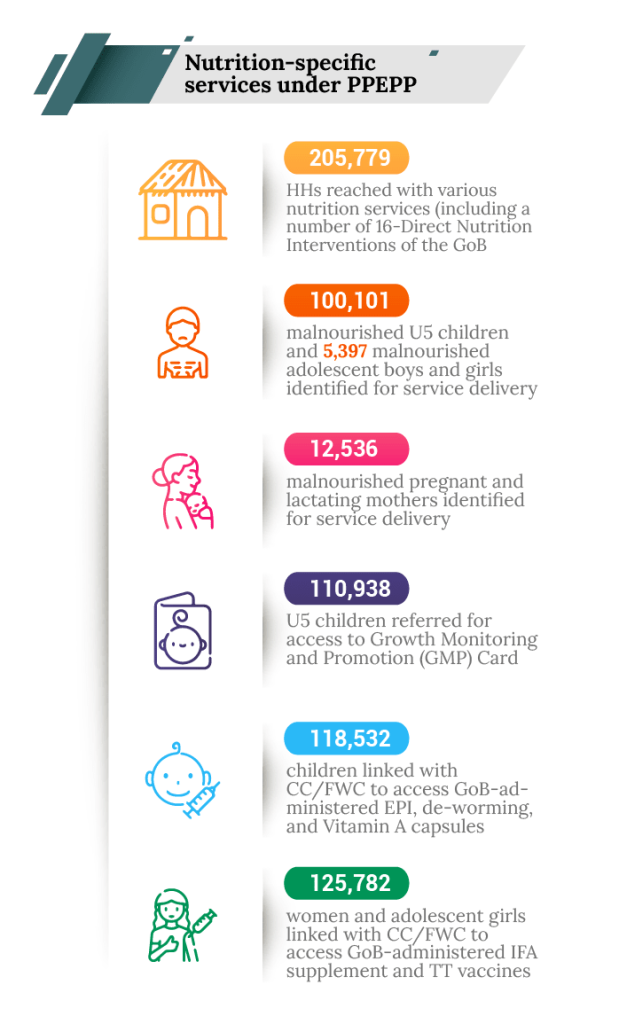
Services around 16 DNIs
Poor health, when left unaddressed, leads to lower productivity and income erosion on the one hand and higher medical cost on the other. PPEPP addresses this in a life-cycle approach.
PPEPP’s nutrition-specific services covers all the 16 DNIs (direct nutrition interventions) promoted by the National Nutrition Services (NNS) of the Bangladesh government. They include Infant and Young Child Feeding (IYCF), micronutrient supplementation, deworming, consumption of nutrient-rich fortified food, management of acute malnutrition and maternal nutrition. We adopt a community-based approach in all our interventions designed based on nutritional need mapping. In integration with the GoB’s nutrition and health system, our referral services and community campaigns ensure access to vaccination, deworming and Vitamin A capsule to prevent various diseases, thus minimising income erosion in the target households.
The project maps the nutritional needs at the target households, especially the children, pregnant and lactating mothers, the elderly, etc. through regular household visits by trained health workers and refer them to the nearest public healthcare facilities. In regular sessions in various platforms formed under the project such as Prosperity Village Committees, Mother and Child Forum, Adolescent Girls/Boys’ Clubs, etc., the project offers counseling on primary health, nutrition, reproductive health, water and sanitation and hygiene.
Access to primary healthcare services

Extreme poor people living in remote areas in Bangladesh often cannot access primary healthcare services due to unavailability of required medicines or specialised doctors at government health facilities. Also, some areas face frequent climate shocks that make the existing health services and facilities inaccessible.
PPEPP project takes the primary healthcare services to the doorsteps of the target population through specialised health camps and satellite clinics across its 145 working unions in 12 districts of Bangladesh. As part of our nutrition-sensitive services, these satellite clinics and health camps are organised in hard-to-reach areas, where healthcare facilities such as Community Clinics and Upazila Health and Family Welfare Centres are nonexistent or the existing facilities are underequipped or understaffed.
Pregnant and lactating mothers, infant and young children, adolescent girls, the elderly and persons with disability are the priority groups who get necessary treatment and referral services through these satellite clinics, specialised health camps (gynaecology, eye camps, etc.) and telemedicine services.
The specialised eye camps provide primary treatments for patients suffering from cataracts, glaucoma, keratitis and retina diseases, nyctalopia and ophthalmia, mostly for elderly people. In coastal region, women and adolescent suffering from reproductive health issues (e.g., uterus diseases, high pressure, abortion) due to salinity get special treatment. A total of 62,396 extremely poor people received primary healthcare services from these health camps and satellite clinics so far.
Linkage building with local health facilities

In Bangladesh, many extremely poor households cannot avail health services from local health facilities due to a lack of awareness and an effective linkage with the service providers. PPEPP project addresses this barrier by establishing this vital linkage with local government and non-government health service providers.
As part of this, the project holds regular advocacy meetings with Community Clinics, Union Health and Family Welfare Centre (UHFWCs) and Civil Surgeon’s office to ensure participant households’ access to government’s health and nutrition services. More than 118,532 children and over 125,782 women and adolescent girls have been linked with CC or UHFWC to access various government services. When necessary, our CNHPs accompany the participants when they visit health facilities to seek treatment.
Muslima Khatun, 28, from Shyamnagar, Satkhira, was linked with a community clinic during her pregnancy. She said, “I received a lot of valuable information about pregnancy and my child’s health and wellbeing from the Community Clinic. They also advised me to eat vitamin-rich food and visit a doctor regularly. This was very helpful.”
Through grassroots advocacy, the project has now representations in the Upazila Nutrition Coordination Committee (UNCC) in different working areas. The 18-member Committee is tasked with planning, implementing, coordinating and evaluating all health and nutrition-related activities at upazila level in line with the national nutrition action plan. Representations in these Committees mean the project can contribute to the successful implementation of UNCC’s health and nutrition strategies.
Social and behaviour change communication for awareness
Many health issues can be prevented through awareness and simple health advice. The project sensitises its members and the larger community about improved nutrition and healthcare through regular household visits and counselling in social platforms.
During individual and group sessions held at households and in different platforms, participants also learn about the basics of food and nutrition, safe water, sanitation, adolescent girls’ nutrition and healthcare, reproductive health, menstrual hygiene and different social issues.
The project also holds demonstrations on ideal food cooking and proper hand washing during sessions at PVCs and Mother and Child Forums to impart knowledge about nutritious food and proper hygiene. The project observes different days such as ‘World Breastfeeding Week’ and ‘Nutrition Week’ to create awareness on the importance of breastfeeding and nutrition.
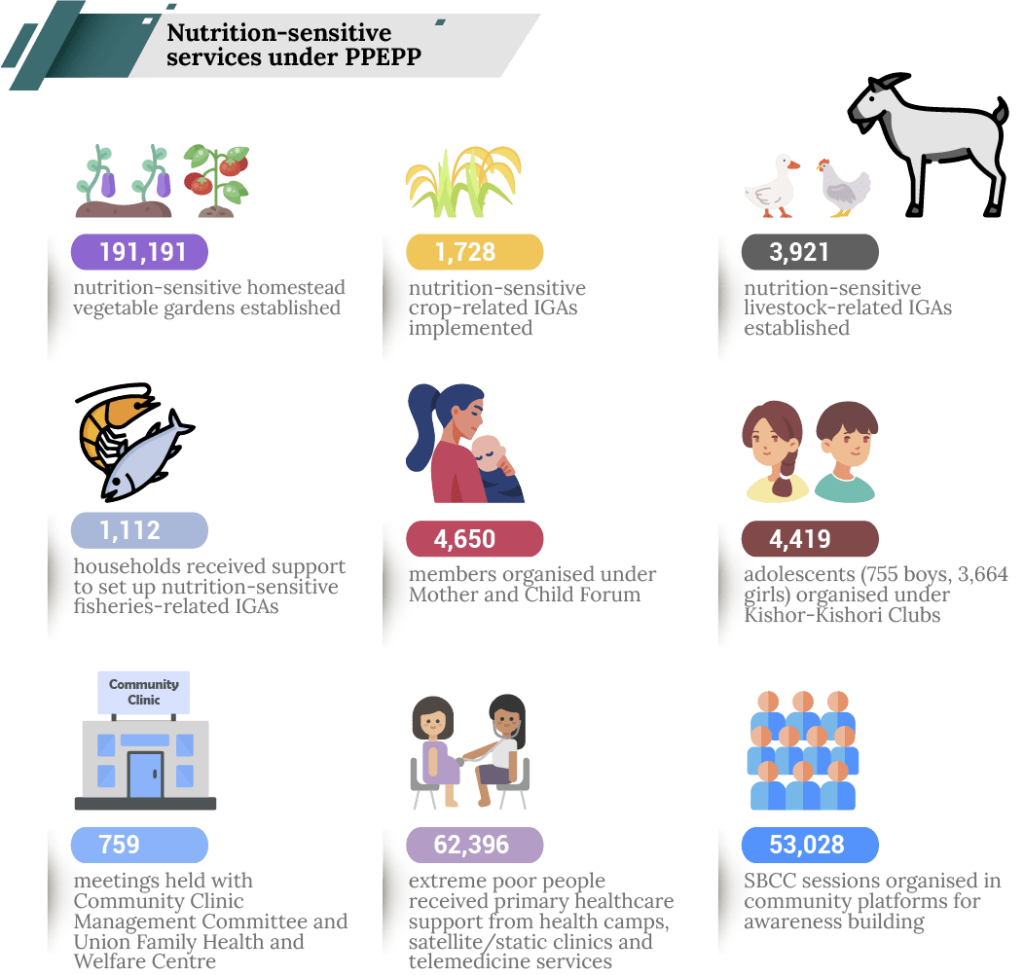
Nutrition-sensitive agriculture: Year-round source of nutrition

Prosperity promotes nutrition-sensitive agricultural interventions such as livestock rearing, fish farming and homestead gardening for all members to make nutritious food more accessible to everyone in the household. The interventions are primarily aimed at meeting the extreme poor households’ need for food and nutrition, but they also support income generation as they can sell the surplus production in the local market.
Apart from homestead gardening at participant households, the project has established 515 ‘Pushti Bagan’ (Nutrition Garden) under Maa o Shishu forums and Kishor-Kishori clubs. Additionally, through grassroots advocacy, the project has established 71 nutrition garden at as many Community Clinics with an aim to encourage community people to grow vegetables on whatever little land they have.
Sumi Akhtar (34), from Galachipa, Patuakhali, is now engaged in fish farming in mini pond and homestead vegetable cultivation.
“The vegetables and fish meet our nutritional needs. I do not need to buy them. I can also sell some in the neighbourhood,” she said.


